Breast Cancer Research in Canada
Breast cancer is a type of cancer that forms in the tissues of the breast. There are many types and it can develop in both women and men, though the prevalence in women is far greater. Breast cancer affects more Canadian women than any other cancer, yet despite its high incidence, it is not the biggest cancer killer. Some 5200 Canadians die of breast cancer each year, a mortality rate that ranks third after lung and colorectal cancers.
Current breast cancer incidence and mortality rates are available through the Canadian Cancer Society, which annually updates these and other statistics. The Canadian cancer registry system allows patterns in cancer incidence and mortality to be tracked across the nation, which makes it an important medical research resource. Registry statistics show a downward trend in the breast cancer mortality rate since the mid-1980s when it peaked at 32 deaths per 100 000 individuals in 1986. This downward trend likely reflects an increase in the early detection of cancers by mammographic screening and the use of increasingly more effective therapies after surgery.
Causes of Breast Cancer
The causes of breast cancer are unknown, although there are known modifiable factors (such as diet, exercise and smoking) and non-modifiable factors (such as genetic predisposition) that influence risk. It is important to recognize that all risk factors do not confer equal risk of getting the disease. For most individuals the biggest risks for breast cancer are gender (being female) and increasing age. Although men do get breast cancer, the incidence rate is very low. Interestingly, breast cancer is one of the few diseases in Canada associated with higher socio-economic status.
Treatment
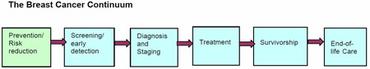
As is the case with most forms of cancer, the path that the breast cancer patient follows is referred to as the breast cancer continuum; it begins with disease detection (hopefully at an early stage), and finishes with end-of-life care. As treatments improve and more women survive longer, breast cancer is beginning to be thought of as a chronic disease and "survivorship" issues are becoming increasingly of interest.
Research activities take place at all stages of the path from diagnosis through treatment to recovery or end-of-life care, and can occur in the lab at a cellular level, in the clinic at a patient level, or in the community at a population level. Basic scientific research "at the bench" examines everything from potential causal pathways, to cellular level responses to treatment. Health services research focuses primarily on access to services and the quality of those services. Clinical research assesses a range of therapeutic interventions from psychosocial therapies to educational or decision aids; from breast reconstruction to cancer treatments, such as surgery, chemotherapy or radiotherapy.
Clinical research frequently uses randomized clinical trials (RCTs) as a methodology. Epidemiological research in breast cancer helps to identify possible risk factors and targets for prevention and often makes use of large, population-based databases, such as cancer registries.
Canada's primary grant-funding agency for breast cancer research is the Canadian Breast Cancer Research Alliance (CBCRA). It represents five agencies, including the government of Canada, with a common vision: to prevent breast cancer, improve survival and enhance the quality of life for those living with breast cancer.
Research
In 1985, October was invoked as breast cancer awareness month with the purpose of promoting discussion and awareness of the disease, and educating women about the importance of early detection. Evidence for the value of the early detection of breast cancer through mammographic screening emerged in the 1980s. As a result, organized screening programs have been established in all provinces and territories in Canada except Nunavut, and screening for breast cancer in women aged 50 and over is widely accepted as a public health intervention that has helped reduce the cancer burden.
Treatment-related research has specific goals for many very specific subgroups of breast cancer patients that include: eliminating the primary tumour and any spread regionally; preventing recurrence locally; preventing distant recurrence; prolonging survival; preventing deaths; reducing symptoms; minimizing side effects and improving quality of life. In Canada, much of this type of research is funded by the Canadian Cancer Society Research Institute (CCSRI) and is implemented by the National Cancer Institute of Canada's Clinical Trials Group (NCIC- CTG).
Over the years NCIC-CTG has published research that has led to important changes in how breast cancer is treated. Four examples of discoveries that have changed practice are:
Women with hormone-sensitive early breast cancer who began the drug letrozole up to five years after completing tamoxifen therapy (an anti-estrogen), had a 69% reduced risk of recurrence compared with women who never took letrozole after completing tamoxifen. This finding is changing how breast cancer survivors are being treated.
The drug Epirubucin is now widely used in Canada to treat women whose breast cancer might recur. This is because Canadian researchers found that in patients with lymph node spread of their disease, an intense drug regimen that included Epirubucin improved survival.
In June 2011, results from a Canadian-led study showed that exemestane, an aromatase inhibitor) reduced risk by 65% in a group of postmenopausal women at risk of breast cancer recurrence.
Findings from another Canadian study looked at how much radiation therapy is needed after lumpectomy (removal of the tumour rather than the entire breast) and showed that shorter radiation therapy schedules were as good as longer treatment schedules in preventing the cancer from returning, with no associated increase in toxicity or side effects.
Personalized Medicine
A futuristic focus in breast cancer research is in designing drugs that target malignant cells by acting on certain mutated genes or the proteins they produce. The trick is to kill cancer cells without harming healthy cells. Canadian researchers are sequencing the DNA of different breast cancer cells to look at their genetic mutations. There has been much discussion about a future in which doctors can routinely analyze the genetic makeup of tumour samples from every cancer patient and determine the specific cancer treatment that would be most helpful to that patient. This is the basis of what has been called "personalized medicine."

 Share on Facebook
Share on Facebook Share on X
Share on X Share by Email
Share by Email Share on Google Classroom
Share on Google Classroom